What is Vitreomacular Traction?
 Throughout life the vitreous (the gel-like substance inside the eye) normally liquefies and gradually separates from the retinal surface. Although this usually results in a complete separation of the vitreous (posterior vitreous detachment), it can sometimes remain stuck to the central macula, the specialized area of the retina that gives us our straight-ahead reading and driving vision. Vitreomacular traction occurs when the adherent vitreous tugs and distorts the macula
Throughout life the vitreous (the gel-like substance inside the eye) normally liquefies and gradually separates from the retinal surface. Although this usually results in a complete separation of the vitreous (posterior vitreous detachment), it can sometimes remain stuck to the central macula, the specialized area of the retina that gives us our straight-ahead reading and driving vision. Vitreomacular traction occurs when the adherent vitreous tugs and distorts the macula

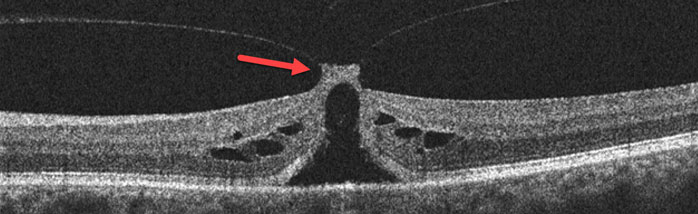
OCT scan (top) of normal macula compared to an eye with vitreomacular traction (bottom)
What are the symptoms of vitreomacular traction?
The mechanical tugging on the macula causes the central vision to be blurred or distorted. In some, the traction can progress to a macular hole. Patients may be completely asymptomatic, especially when the other eye sees normally.
How is vitreomacular traction diagnosed?
You can’t diagnose vitreomacular traction by looking in the mirror since your eye will look and feel normal. The diagnosis is made with a thorough retinal examination through a dilated pupil and confirmed with OCT scanning.
What treatments are available for vitreomacular traction?
Observation.
Treatment is often not necessary since many patients remain asymptomatic. Even with significant symptoms observation is often initially recommended since the traction can spontaneously release in up to 50% of cases. Treatment should be considered for those whose distortion, vision loss, and decreased depth perception make their daily activities such as reading and driving difficult.
Pneumatic vitreolysis.
A painless in-office injection of a gas bubble into the vitreous, similar to pneumatic retinopexy, successfully resolves vitreomacular traction in about 80% of patients.
Jetrea.
Laminin, fibronectin and collagen make the vitreous stick to and distort the macula. Jetrea dissolves this biologic glue, releasing the adherent vitreous in up to 50% of cases. Although a successful injection avoids vitrectomy surgery, it can rarely cause temporary vision loss. Your doctor will discuss all the risks vs benefits if they feel this might be a good option for you.
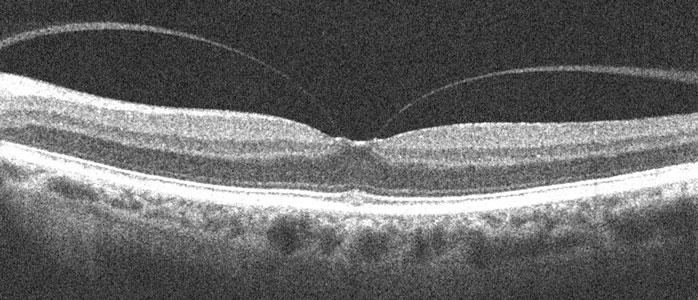
Vitreous traction tenting up the central macula
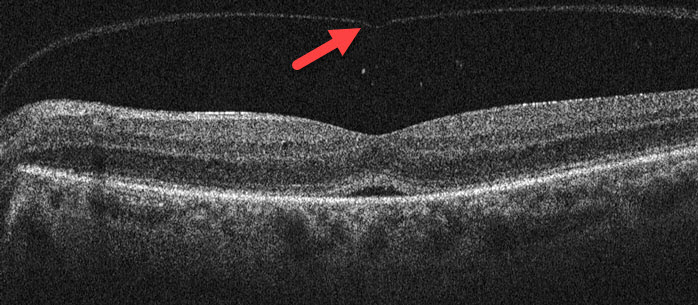
The vitreous completely separated following Jetrea
Vitrectomy surgery.
Vitrectomy surgery is done in an operating room under local anesthesia. This advanced microsurgical technique restores vision by peeling the adherent vitreous from the macular surface, allowing the underlying macula to smooth out and function more normally. Patients go home immediately following surgery. There is usually minimal to no pain, except for minor irritation.
Patients usually notice improved vision with decreased distortion within several weeks to months following vitrectomy although it may take much longer for maximal vision to return. The major surgical side-effect is a cataract, with many patients requiring cataract surgery within a year or two of vitrectomy. There is also a very small chance for secondary retinal detachment or infection.
View more retina images at Retina Rocks, the world’s largest online multimedia retina image library and bibliography repository.



