What is anterior ischemic optic neuropathy (AION)?
The optic nerve represents the cable connecting the eye to the brain, carrying all of the information from the retina that we need to see. As the nerve enters the back of the eye, it receives its nutrients from a few tiny blood vessels. When there is a problem with these blood vessels, either from inflammation or a lack of blood supply, the optic nerve becomes sick and damaged.
Who gets AION?
About 10% of cases are caused by giant cell (temporal) arteritis, an inflammation of larger blood vessels usually found in older individuals. This is called arteritic AION. Patients often have symptoms of pain with chewing, temporal headaches, weight loss, and weakness. If untreated, the other eye is often affected.
About 90% of cases are due to other causes (non-arteritic AION). This is more common in patients with small optic nerves (an anatomic variant), high blood pressure, diabetes, arteriosclerosis, high cholesterol, and sleep apnea. Certain medications used to treat erectile dysfunction and cardiac arrhythmias (amiodarone) are associated with an increased risk of AION. Patients with non-arteritic AION are also at an increased risk for a stroke.
What are the symptoms of AION?
Most patients will notice painless central and/or peripheral vision loss in one eye, usually upon waking in the morning. The symptoms are often described as a large “black spot” in the vision that does not move. The vision loss can be mild to severe.
How is AION diagnosed?
A detailed history by your eye doctor followed by a dilated eye exam will help in the diagnosis. Bloody swelling of one optic nerve is usually found. A brain MRI may be ordered to rule out other causes of a swollen nerve. Blood work is often ordered to rule out giant cell arteritis.
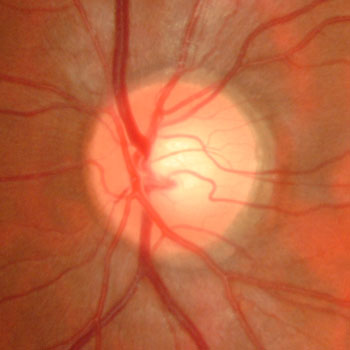
Normal optic nerve
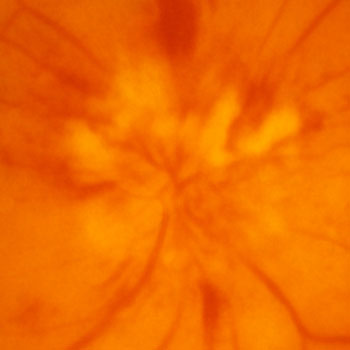
Swollen optic nerve with AION
How is AION treated?
Unfortunately, there is no effective treatment for AION. The initial vision loss is often permanent although there may be some improvement over the first few months. The optic nerve swelling often resolves over weeks to months, turning the normal pink nerve into a permanently damaged pale yellow nerve. A visual field is often useful in evaluating how much damage has occurred and in monitoring for further changes. The risk of a similar event happening in the other eye for non-arteritic AION varies based on what individual risk factors are present, ranging from 12% to 40%.
Patients with arteritic AION need to be emergently treated with high-dose prednisone due to the extremely high risk of the other nerve being affected. A biopsy of a temporal artery is often obtained to confirm this diagnosis. Treatment, which is often necessary for months to years, is usually coordinated with the patient’s medical doctor or rheumatologist. Although steroids do nothing to restore vision in the affected eye, they are highly effective in preventing vision loss in the other eye.
View more retina images at Retina Rocks, the world’s largest online multimedia retina image library and bibliography repository.



