What are Retinitis Pigmentosa (RP) and Inherited Retinal Diseases (IRDs)?
Inherited retinal diseases (IRDs) are a group are rare potentially blinding genetic retinal disorders associated with over 260 different genetic mutations. Many of these disorders, which affect about 200,000 people in the United States, are generally lumped together under the single term of retinitis pigmentosa (RP). RP can appear in a person with no other affected family members, as a dominant trait (an affected individual has a 50% chance for each child getting the disease), as a recessive trait (each parent carries the gene but does not show any signs of RP themselves), or as sex-linked trait (passed from a usually unaffected mother to half of her sons who are usually affected and to half of her daughters who are usually unaffected carriers).
RP primarily affects the rods and cones, the retinal cells responsible for capturing the light images in our eyes. The genetic defect in these cells causes the outer retinal layers to atrophy, with the pigmented layer of cells below the retina (the retinal pigment epithelium, or RPE) typically migrating into the retina in a bone-spicule pattern. There is an increased risk for cataracts and cystoid macular edema. Most patients have variable symptoms of night blindness, difficulty adjusting to a dark environment, side vision loss, and central vision loss.
How is RP diagnosed?
RP is usually diagnosed during a dilated ocular examination. Most affected patients will have a typical appearance of bone spicules, a pale optic nerve, and narrowed retinal vessels, OCT scanning, fluorescein angiography, and electroretinogram (ERG) are often used to confirm the diagnosis. Visual field testing typically shows mild to severe side vision loss that can result in ‘tunnel vision.’
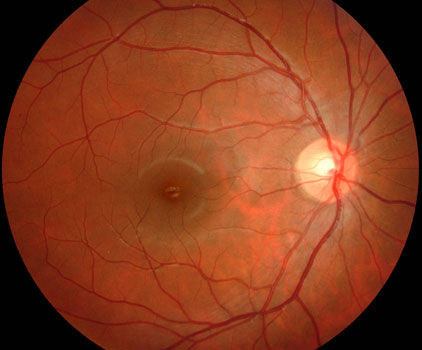
Normal macula
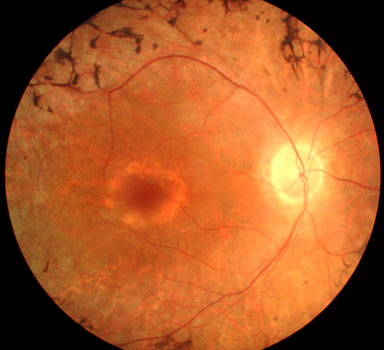
Retinitis pigmentosa with loss of macular pigment and black bone spicules more peripherally
How is RP treated?
Patients with IRDs and RP need to be examined regularly since both cataracts and macular edema are often treatable. Vitamin A palmitate (15,000 international units) has been shown to possibly slow the disease progression and may be recommended for some.
We may recommend that you see a specialist for a low vision examination. Magnifying lenses or other devices can be prescribed to help with reading and other central vision tasks. For those living in the Kentuckiana and Northern Kentucky areas, the Kentucky Office for the Blind, the Cincinnati Association for the Blind and Visually Impaired, Free Kentucky Talking Book Library Service, and the American Printing House for the Blind offer a myriad of services and resources to help those with vision loss function better and remain independent. Radio Eye is a non-profit 24-hour radio service that broadcasts the reading of current newspapers and other everyday literature, offering greater independent living to people who are blind, visually impaired or physically handicapped. Radio Eye radio listeners hear the reading of dozens of newspapers, magazines, health materials, grocery ads and much more. The audio stream can be accessed on a special (free) Radio Eye radio, on Library Channel 20 on Lexington Insight Cable TV, in area homes and hospitals, as well as on their website. Lighthouse Guild is a leading nonprofit vision and healthcare organization, with a long-standing heritage of addressing the needs of people who are blind or visually impaired, including those with multiple disabilities or chronic medical conditions. Through the integration of vision and healthcare services and the expansion of access through education and community outreach, their innovative and comprehensive approach helps people achieve and maintain the highest possible level of function and independence. Many patients are able to maintain a normal active life, although some will develop legal blindness due to peripheral or central vision loss. Low vision services or referral to the Department for the Blind can help severely affected individuals to maintain their independence.
In 2018 gene therapy became a reality for some patients with certain sub-types of IRDs caused by a defect in the RPE65 gene which produces a protein that is vital to normal vision. RPE65 mutations are found in 8% to 16% of patients with Leber’s congenital amaurosis and 1% to 3% of patients with RP. Luxturna gene therapy is a one-time surgery where normal RPE65 genes are injected below the retina and get incorporated into the patient’s own cells which then produce the normal RPE65 protein. Patients must have viable retinal cells in order for treatment to be effective.
View more retina images at Retina Rocks, the world’s largest online multimedia retina image library and bibliography repository.



