What is Pars Planitis?
Pars Planitis is an inflammation of the pars plana, the tissue that lines the inside front portion of the eye. White inflammatory material accumulates overlying the pars plana, peripheral retina and vitreous. One or both eyes can be affected.
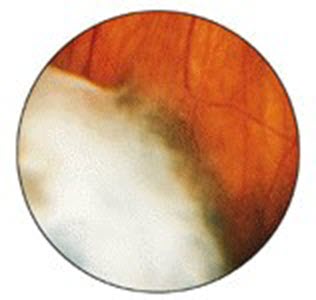
White inflammatory material overlying the peripheral retina
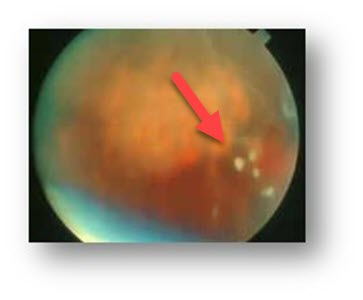
White clumps of vitreous floaters
Mild cases can be totally asymptomatic. As the inflammation becomes more extensive, inflammatory debris can extend into the vitreous causing floaters. The macula can swell (cystoid macular edema) resulting in central blurriness. Occasionally inflammation can spill into the front portion of the eye (iritis) causing redness, pain, and sensitivity to light (photophobia).
The inflammation waxes and wanes over many years and usually becomes inactive over several decades. Pars planitis generally occurs in young, healthy women. It has no associated systemic diseases, although similar findings can occur with sarcoidosis, Lyme disease, and multiple sclerosis.
How is pars planitis diagnosed?
Pars planitis is diagnosed by your eye doctor with a dilated retinal examination. The diagnosis can be subtle since the pars plana is a difficult area of the eye to examine. Cystoid macular edema is detected with OCT scanning and fluorescein angiography.
How is pars planitis treated?
Mild asymptomatic inflammation is observed. Steroid injections are given as needed for symptomatic floaters or cystoid macular edema. Steroid eye drops are used for iritis. Cryotherapy to the pars plana for more severe and persistent inflammation is often curative. Rarely vitrectomy surgery is necessary to remove non-clearing vitreous floaters. Most patients will retain excellent vision.
View more retina images at Retina Rocks, the world’s largest online multimedia retina image library and bibliography repository.



